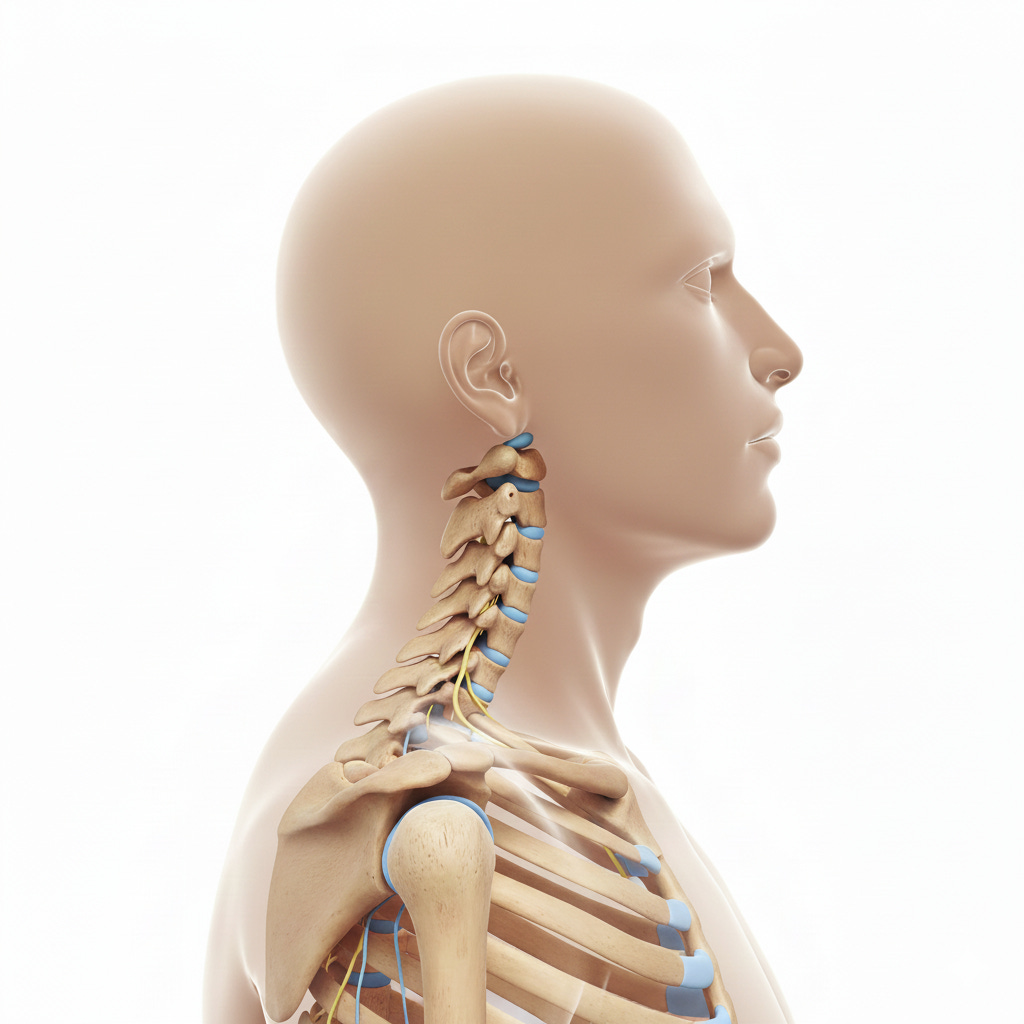
Beyond the Pill: How Physical Therapy Can Offer Lasting Relief for Migraines
For individuals battling migraines, the search for a meaningful solution often extends beyond acute medication. Migraines are complex, debilitating neurological events that involve central sensitization, often leaving patients in cycles of pain, photophobia, and nausea. While they are classified as a primary headache disorder, a significant and often overlooked component lies in the musculoskeletal and mechanical stresses of the neck and upper back.
As a physical therapist integrating holistic medicine, my focus is on this critical intersection: addressing the physical triggers and teaching the central nervous system to lower its alarm levels. This article dives into the evidence-based neuroanatomy and specific PT interventions that can offer lasting, preventative relief by treating the root mechanical and neurological contributors.
The Evidence: Anatomical and Neural Overlap
To understand why a neck problem can feel like a head problem, we must explore the anatomical bridge. Research confirms a high rate of overlap between migraines and headaches originating from the neck, known as cervicogenic headaches [Côté et al., 2019; Jull et al., 2007]. Many patients experience a hybrid, where musculoskeletal factors act as a potent trigger for a full-blown migraine.
The Trigemino-Cervical Nucleus (TCN)
The key to this connection is the Trigemino-Cervical Nucleus (TCN)—a central hub located in the brainstem and upper cervical spinal cord.
Trigeminal Input: The primary input to the TCN comes from the trigeminal nerve (Cranial Nerve V), which supplies sensation to the face, skull, and major pain-sensitive structures inside the head, and is central to the migraine process.
Cervical Input: The upper cervical spinal nerves, specifically C1-C3, which supply the muscles, joints, and ligaments of the upper neck, also terminate directly in the TCN [Watson & Drummond, 2014].
This means the TCN acts as a convergence point. When the tissues in the upper neck are stressed, stiff, or inflamed due to poor posture, joint dysfunction, or muscle tension, the C1-C3 nerves send distress signals to the TCN. The brain struggles to differentiate the source of these signals, often interpreting them as being from the trigeminal system—resulting in pain perceived in the head or face [Watson & Drummond, 2014]. By treating the neck, we are directly modulating a key pain-processing center in the brainstem.
Postural Stress and Muscle Fatigue
The modern epidemic of forward head posture creates chronic mechanical stress.
The head weighs approximately 10 to 12 pounds (4.5 to 5.5kg). For every inch the head moves forward, the force on the neck muscles can increase by about 10 pounds. This sustained loading leads to:
Muscle Ischemia: The suboccipital muscles and upper trapezius become chronically tense, restricting blood flow and leading to a buildup of metabolic waste that irritates local nerve endings.
Joint Restriction: Sustained poor posture can lead to hypomobility (stiffness) in the C1-C3 facet joints, which directly feeds into the TCN [Sterling et al., 2001].
Physical Therapy Interventions: Restoring Mechanical Balance
Physical therapy is a systematic approach to restoring normal biomechanics and reducing the noxious input flowing into the TCN. This is achieved through a two-pronged strategy: hands-on techniques and specific therapeutic exercise.
1. Manual Therapy: Desensitizing the System
Manual techniques are used to immediately reduce tension and restore joint function [Jull et al., 2007; Sterling et al., 2001].
Cervical Joint Mobilization: This involves rhythmic, controlled movements applied to stiff upper cervical joints (C1-C3). The goal is not just to improve mobility, but also to trigger a neurophysiological effect: the gentle movement stimulates joint receptors that can inhibit pain signals passing through the TCN [Sterling et al., 2001].
Soft Tissue Release & Trigger Point Deactivation: Techniques like ischemic compression or myofascial release are used on trigger points in the upper trapezius and suboccipital muscles. Releasing these knots reduces the local irritation and muscle-related pain input that feeds the headache cycle.
2. Therapeutic Exercise: Building Resilience
While manual therapy provides immediate relief, therapeutic exercise is the key to long-term prevention. It creates structural and muscular changes that withstand the stressors of daily life [Jull et al., 2007; Falla, 2004].
Deep Neck Flexor (DNF) Strengthening: These small muscles (e.g., longus colli, longus capitis) are the primary stabilizers of the cervical spine. In migraine and headache sufferers, the DNFs are often weak or inhibited. Specific low-load exercises (like the chin tuck) target these muscles, teaching them to hold the head in a stable, neutral position, which significantly offloads the hyperactive superficial muscles [Falla, 2004].
Scapular and Postural Correction: Strengthening the middle and lower trapezius muscles is critical. When the muscles supporting the shoulder blades are weak, the shoulders round forward, leading to a compensatory forward head posture. Strengthening these muscles helps anchor the upper back and maintain the thoracic extension necessary for a pain-free neck. Simple prone Y or cobra with “prone Y” is a great tool.
Holistic Integration: Modulating the Central Nervous System
True healing requires integrating the physical changes with neurological regulation. Migraines are fundamentally a disorder of central sensitization, where the nervous system is chronically set to a high-alert state [Maizels, 2007]. The holistic approach teaches the body how to turn down the volume on pain signals.
Vagal Nerve Toning and Stress Resilience
The vagus nerve is the longest cranial nerve and the primary component of the parasympathetic nervous system (PNS—the “rest and digest” mode). Stimulating the vagus nerve is a direct way to counteract the sympathetic “fight or flight” response, which is often heightened during chronic stress and pain states.
Diaphragmatic Breathing: This is the most accessible method of vagal toning. By inhaling deeply into the abdomen and exhaling slowly and fully, you mechanically stimulate the vagus nerve, promoting a shift to the PNS. Consistent practice (even 5 minutes, three times a day) helps the entire nervous system become less reactive over time.
Mindfulness and Body Awareness: Integrating practices like gentle yoga or mindful walking helps patients notice when they are unconsciously bracing, tightening their neck, or adopting poor posture. This awareness allows them to consciously intervene and release tension before it escalates into a trigger.
Consistency Over Intensity: The Energetic Shift
Holistic healing emphasizes the power of consistency—the regular, small habits that rewire the nervous system. The goal is to regulate energy and reduce the body’s overall “allostatic load” (the wear and tear on the body due to chronic stress). Exercise is not just for muscles; it’s a proven intervention for emotional regulation, improving sleep quality, and elevating mood, all of which indirectly reduce the neurological burden that can trigger a migraine [Maizels, 2007].
Conclusion
Physical therapy offers a robust, evidence-based pathway to lasting migraine relief by intervening at the crucial Trigemino-Cervical Nucleus. By restoring the biomechanical integrity of the upper neck through manual therapy and targeted exercise, we reduce the noxious input that drives headache pain.
Coupled with a holistic focus on vagal toning and stress resilience, this dual approach empowers you to move beyond simply managing symptoms. It allows you to transform your nervous system’s response, leading to a state of lower pain sensitivity, greater confidence, and true long-term wellness.
References
Côté, P., et al. (2019). The global problem of headache: a narrative review of the role of physical therapy in its management. Musculoskeletal Science and Practice.
Falla, D. (2004). Deep cervical flexor muscle training is effective in reducing chronic neck pain. Clinical Biomechanics.
Jull, G., Behrstock, B., & Behrstock, V. (2007). A randomized controlled trial of exercise and manipulative therapy for cervicogenic headache. Spine.
Maizels, M. (2007). The role of the nervous system in headache and migraine. The Journal of Head and Face Pain.
Sterling, M., et al. (2001). The contribution of the cervical spine to headache. Journal of Musculoskeletal Pain.
Watson, D. H., & Drummond, P. D. (2014). Cervical referral of head pain in migraineurs: effects on the nociceptive blink reflex. Pain.